Nahrungsmittelallergie: Was ist das?

Nahrungsmittelallergien werden häufiger vermutet, als sie tatsächlich auftreten. Dennoch steigt sie Anzahl der Betroffenen, insbesondere bei Kindern. Was sind die Ursachen, wie sehen typische und untypische Symptome aus und was ist anders bei Kindern? Mehr zu Diagnose und Therapieansätzen finden Sie hier:
Autor: Dr. med. Anna Eger
Was ist eine Nahrungsmittelallergie?
Wenn Menschen bestimmte Nahrungsmittel nicht vertragen, bezeichnet man dies als “Nahrungsmittelunverträglichkeit“. Es gibt allerdings unterschiedliche Formen von Nahrungsmittelunverträglichkeiten. Zum einen gibt es „allergisch bedingte Nahrungsmittelunverträglichkeiten“, oder auch „Nahrungsmittelallergien“. Zum anderen kann es zu „nicht allergisch bedingten Nahrungsmittelunverträglichkeiten“ kommen, die auch als Nahrungsmittelintoleranzen bezeichnet werden.
Nahrungsmittelallergien (NMA) und Nahrungsmittelunverträglichkeiten (NMU): Was ist der Unterschied?
Nahrungsmittelunverträglichkeit ist der Oberbegriff für verschiedene Symptomkomplexe, die durch Nahrungsmittel ausgelöst werden. Man unterscheidet zwischen strukturellen und funktionellen Nahrungsmittelunverträglichkeiten. Dabei liegt den funktionellen Nahrungsmittelunverträglichkeiten eine Funktionsstörung des Immunsystems oder verschiedener Enzyme bzw. Proteine zugrunde. Die Nahrungsmittelallergie ist eine Form der Nahrungsmittelunverträglichkeit, die nicht toxisch, aber immunologisch bedingt ist. Es gibt IgE- und nicht-IgE-vermittelte Nahrungsmittelallergien. Nicht zu verwechseln sind Nahrungsmittelallergien mit den Nahrungsmittelintoleranzen. Diese sind ebenfalls nicht toxisch, aber auch nicht immunologisch bedingt. Schließlich gibt es als letztes noch die toxischen Nahrungsmittelunverträglichkeiten, zu denen zum Beispiel die Lebensmittelvergiftung zählt.
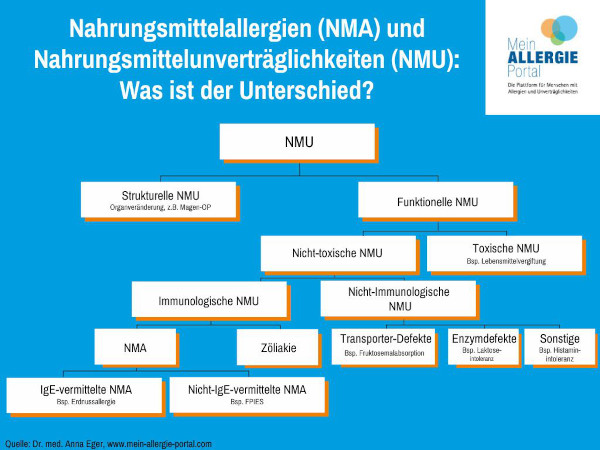 Was ist der Unterschied zwischen Nahrungsmittelallergien und nicht allergischen Nahrungsmittelunverträglichkeiten?
Was ist der Unterschied zwischen Nahrungsmittelallergien und nicht allergischen Nahrungsmittelunverträglichkeiten?
Welche Nahrungsmittelallergien gibt es?
Man kann Nahrungsmittelallergien in 4 verschiedene Gruppen einteilen, abhängig von ihrem Entstehungsmechanismus:
- IgE-vermittelte Nahrungsmittelallergie
- Zytotoxische Nahrungsmittelallergie
- Immunkomplex-bedingt Nahrungsmittelallergie
- T-Zell-vermittelte Nahrungsmittelallergie
| Klassifikation Nahrungsmittelallergien nach Entstehungsmechanismus | ||
| Gruppe | Merkmale/Besonderheiten | Beispiele |
| IgE-vermittelt | Lösliche Antigene binden an den spezifischen IgE-Rezeptoren von Mastzellen, woraufhin verschiedene Botenstoffe freigesetzt werden (zum Beispiel Histamin) | Typ A – Kuhmilchallergie Typ B – Orales Allergiesyndrom Typ C – Fleischallergie |
| Zytotoxische NMA | Durch Antikörper vermittelte zytotoxische Reaktion, bei der Zellen abgetötet werden | Für NMA eher unerheblich, eher durch Medikamente ausgelöst |
| Immunkomplex-bedingte NMA | Durch IgG-Antikörper vermittelte Bildung von Immunkomplexen und Freisetzung von Botenstoffen aus Mastzellen und anderen Zellen | Für NMA eher unerheblich, eher durch bakterielle Strukturen oder Schimmelpilze ausgelöst |
| T-Zell-vermittelte NMA | Durch Antigene vermittelte Reaktion der T-Zellen des Immunsystems, welche wiederum zur Freisetzung von Histamin aus Mastzellen u.a. führt. | Ekzemverschlechterung, hämtogenes Kontaktekzem, tritt verzögert nach Kontakt/ Verzehr beispielsweise von Weizen auf |
| Quelle: Dr. med. Anna Eger, www.mein-allergie-portal.com |
||
Die IgE-vermittelten Nahrungsmittelallergien werden nochmals in 3 Untergruppen untergliedert:
1. Typ A -etwa 5 bis 10 Prozent
Die Sensibilisierung erfolgt über den Magen-Darm-Trakt. Sie tritt im Säuglingsalter auf und bildet sich bei etwa 80 Prozent der Patienten im Laufe des Lebens zurück. Zu ihnen zählen die Kuhmilchallergie sowie die Allergie gegen Ei, Fisch, Erdnuss, Haselnuss und Soja.
2. Typ B - etwa 75 Prozent – sekundäre Form
Die Sensibilisierung bei dieser Form erfolgt über den Atemweg, indem Allergene aus der Luft IgE ausbilden, die eine Kreuzreaktion mit ähnlichen Proteinen in Nahrungsmitteln hervorrufen. Häufig sind es nur leichte Beschwerden wie zum Beispiel im Rahmen eines oralen Allergiesyndroms.
3. Typ C - etwa 15 Prozent – primäre Form
Diese Form betrifft meist erwachsene Frauen, bei denen bislang keine Atopie vorlag. Die Sensibilisierung findet im Magen-Darm-Trakt statt. Die Allergene sind relativ verdauungsstabile Proteine, wie zum Beispiel Krustentiere, Fisch, Ei, Milch, Fleisch oder pflanzliche Allergene wie Erdnuss, Kiwi, Feige, Karotte oder Curry.
Auf welche Lebensmittel kann man allergisch reagieren?
Prinzipiell kann man auf alle Lebensmittel allergisch reagieren. Es gibt jedoch Nahrungsmittel, auf die häufiger allergische Reaktionen auftreten und solche, die selten für allergische Reaktionen verantwortlich sind. Im Folgenden werden einige typische allergene Nahrungsmittel genannt.
Was sind die häufigsten Nahrungsmittelallergien?
Diese Nahrungsmittelallergien kommen häufig vor:
- Allergie auf Kuhmilch
- Allergie auf Weizen
- Allergie auf Hühnerei
- Allergie auf Soja
- Allergie auf Baumnüsse, wie zum Beispiel Haselnüsse
- Allergie Hülsenfrüchte wie Erdnüsse
- Allergie auf Samen, wie zum Beispiel Sesam oder Leinsamen
- Allergie auf Fleisch
- Allergie auf Geflügelfleisch
- Allergie auf Fisch
- Allergie auf Meeresfrüchte, Krustentiere
- Allergie auf Obst, wie zum Beispiel Kiwi
- Allergie auf Zerealien
Gibt es besonders allergene Lebensmittel?
Die Art der Lebensmittel, die besonders allergen sind, unterscheiden sich bei Kindern und Erwachsenen etwas. Für Kinder sind besonders Hühnereiweiß- und Milcheiweißprodukte relevant, sowie Soja und Erdnuss. Die Erdnussallergie ist in den letzten Jahrzehnten dreimal häufiger geworden. Bei Erwachsenen sind vor allem Sellerie, Karotte, Nüsse, Kern- und Steinobst sowie Krusten- und Schalentiere besonders allergen. Weizen gilt sowohl für Kinder als auch für Erwachsene als potentiell besonders allergen.
Seltenere Nahrungsmittelallergien
Es gibt neben den häufigeren Nahrungsmittelallergien auch seltenere Formen. Eine Sonderform der Nahrungsmittelallergie ist die zum Beispiel die WDEIA, die Weizenabhängige anstrengungsinduzierte Anaphylaxie.
Daneben gibt es die eosinophile Ösophagitis (EoE) und das Food Protein Induced Enterocolitis Syndrome [FPIES], auf Deutsch Nahrungsprotein induziertes Enterokolitis-Syndrom.
Eosinophile Ösophagitis (EoE)
Die Eosinophile Ösophagitis ist eine chronische Schleimhautentzündung der Speiseröhre, die immunologisch vermittelt wird und durch eine Infiltration der Schleimhaut mit sogenannten eosinophilen Granulozyten – das sind bestimmte Immunzellen – gekennzeichnet ist. Etwa 50 von 100.000 Einwohner leiden an dieser Erkrankung, wobei Männer dreimal häufiger als Frauen betroffen sind und der Erkrankungsgipfel zwischen dem 30. und 50. Lebensjahr liegt. Die genauen Ursachen sind unbekannt. Man weiß jedoch, dass Nahrungsmittel- oder Aeroallergene eine Entzündungsreaktion in Gang setzen, die über bestimmte Zytokine Eosinophile und Mastzellen aktivieren.
Food Protein Induced Enterocolitis Syndrome [FPIES]
FPIES, auf Deutsch Nahrungsmittelprotein-induziertes Enterokolitis-Syndrom, ist eine seltene und unter Umständen sehr plötzlich auftretende und schwer verlaufende Reaktion auf Nahrungsmittel, die nicht IgE-vermittelt ist. Meistens sind junge Säuglinge betroffen. Bisher ist über den genauen Entstehungsprozess nicht so viel bekannt.
Die häufigsten Auslöser für das FPIES sind:
- Milch(produkte)
- Soja
- Getreide
Seltener sind folgende Nahrungsmittel für die Reaktion verantwortlich:
- Reis
- Hafer
- Fisch
- Ei
Wie häufig sind Nahrungsmittelallergien?
Die Häufigkeit von Nahrungsmittelallergien wird überschätzt. Das hängt u.a. auch damit zusammen, dass die Begrifflichkeiten von Unverträglichkeit und Allergie häufig falsch verwendet werden. So wird zum Beispiel eine Laktoseintoleranz häufig mit einer Allergie gegen Milch gleichgesetzt. Es gibt auch nur begrenzt Studien über die Prävalenz, also Häufigkeit, von Nahrungsmittelallergien. Allgemein kann man sagen, dass die Häufigkeit regional sehr unterschiedlich ist und in einigen Ländern die Nahrungsmittelallergien deutlich zugenommen haben. Es gibt Angaben zwischen 3,7 Prozent bei Kindern und 4,7 Prozent bei Erwachsenen, wobei der Anteil Frauen über doppelt so hoch ist.
Kann man plötzlich eine Nahrungsmittelallergie bekommen?
Eine Nahrungsmittelallergie kann man plötzlich in höherem Lebensalter bekommen, auch wenn man bisher keinerlei Beschwerden beim Verzehr eines bestimmten Lebensmittels hatte. Eine IgE-vermittelte Allergie vom Typ B oder C, also die sekundäre oder primäre Form, entwickelt sich im Laufe des Lebens entweder auf dem Boden einer Sensibilisierung über die Atemwege durch beispielsweise Pollen oder über den Magen-Darm-Trakt.
Kann man multiple Nahrungsmittelallergienhaben?
Es ist natürlich möglich, dass man auf mehrere Allergene mit einer allergischen Reaktion reagiert. Immerhin leiden etwa 30 Prozent der Nahrungsmittelallergiker nicht nur unter einer, sondern unter multiplen Nahrungsmittelallergien. Man muss bedenken, dass man bei herkömmlicher Ernährung innerhalb von 24 Stunden etwa 120 verschiedene Nahrungsmittelallergene zu sich nimmt. Für multiple Nahrungsmittelallergien spielen auch die Kreuzallergien eine wichtige Rolle.
Um welche Reaktionstypen handelt es sich bei einer Lebensmittelallergie? Typ 1, 2, 3 oder 4?
Die überwiegende Anzahl der Nahrungsmittelallergien sind nach der Einteilung von Allergien nach Coombs und Gell dem Typ 1 zuzuordnen. Diese wird über IgE-Antikörper vermittelt und wird auch als Sofort-Typ-Allergie bezeichnet. Das heißt, die Reaktion tritt unmittelbar nach dem Verzehr des allergenen Nahrungsmittels auf. Es gibt aber seltenere Nahrungsmittelallergien vom Typ 2 bis 4, welchen ein anderer Mechanismus zugrunde liegt und die verzögert auftreten.
Nahrungsmittelallergien: Was ist die Ursache?
Zu den allergischen Nahrungsmittelunverträglichkeiten zählen solche, bei denen das Immunsystem beteiligt ist. Die Mehrzahl der Nahrungsmittelallergien wird durch Immunglobulin E-Antikörper verursacht. Immunglobuline E (IgE) sind Antikörper, die sich spezifisch gegen ein bestimmtes Allergen richten. Bei Allergikern kommt es nach Kontakt mit Allergenen zu einer gesteigerten Produktion im Sinne einer Überreaktion des Immunsystems. Die Reaktion zeigt sich meist unmittelbar nach Kontakt mit dem Allergen, manchmal auch bis zu zwei Stunden danach. Letztendlich kann man nicht mit 100prozentiger Sicherheit sagen, was die Ursachen von Nahrungsmittelallergien sind, es gibt jedoch Hypothesen und Hinweise.
Genetische Veranlagung und Nahrungsmittelallergien
Wie bei vielen Erkrankungen spielt die genetische Veranlagung eine ziemlich große Rolle für die Entstehung und Ausprägung einer Nahrungsmittelallergie. Bestehen bereits in der Familie atopische Erkrankungen oder treten gehäuft Allergien auf, dann steigt das Risiko, an einer Nahrungsmittelallergie zu erkranken, an.
Die Hygiene-Hypothese und Nahrungsmittelallergien
Es gibt mehrere Theorien zur Zunahme von Allergien. Da ist zum einen die Hygiene-Hypothese. Die Hygiene-Hypothese geht davon aus, dass unser Immunsystem unterfordert ist, weil wir heutzutage immer seltener mit schweren Infektionskrankheiten wie etwa Tuberkulose konfrontiert werden. Aufgrund dieser Unterforderung begeht das Immunsystem einen „Irrtum“, denn es stürzt sich auf im Grunde harmlose Allergene in Pollen- oder Hausstaubmilben und stuft sie fälschlicherweise als „gefährlich“ ein.
Umweltfaktoren und Nahrungsmittelallergien
Auch Umweltfaktoren könnten bei der Zunahme von Allergien eine Rolle spielen. Die Umweltverschmutzung nimmt zu und nicht ohne Grund ist die Zahl der Allergiker in den Städten deutlich höher als auf dem Land. In den Städten findet man auf den Pollen Rußpartikel, die die Allergenität der Pollen erhöhen. Das Immunsystem wertet die mit Rußpartikeln besetzten Pollen wie ein Bakterium und greift an – die Folge: Allergische Symptome.
Das Mikrobiom und Nahrungsmittelallergien
Zunehmend rückt auch die Rolle des Darms bei der Entstehung von Nahrungsmittelallergien in den Fokus. Die Forschungen dazu stecken aktuell noch in den Kinderschuhen. Es erhärten sich aber die Hinweise darauf, dass es einen Zusammenhang zwischen den Mikroorganismen im Darm und Veränderungen im Immunsystem gibt, die eine Nahrungsmittelallergie hervorrufen können. Möglicherweise könnte ein gesunder Darm vor Allergien schützen.
Nahrungsmittelallergien: Wie sensibilisiert man sich?
Festzustehen scheint, dass es bei den Nahrungsmittelallergien, den IgE-vermittelten Nahrungsmittelunverträglichkeiten, nicht nur eine Möglichkeit gibt, eine Sensibilisierung zu erwerben. Es gibt zwei bedeutsame Sensibilisierungswege bei der Nahrungsmittelallergie, zum einen die Aufnahme über die Nahrung, das heißt die orale Aufnahme, und zum anderen die Exposition über die Haut. Zumindest kann letztes für manche Nahrungsmittel als bedeutsamer Sensibilisierungsweg angenommen werden. Weiter gibt es auch Hinweise darauf, dass die Möglichkeit besteht, sich über die Atemwege, das heißt über die Inhalation von Nahrungsmittelproteinen, zu sensibilisieren. Zwar steht für den Sensibilisierungsweg über die Atemwege nicht fest, wie bedeutsam er ist. Die Atemwegsschleimhäute sind jedoch ein Teil des Immunsystems und man weiß, dass allergische Reaktionen auf Nahrungsmittel über die Atemwege ausgelöst werden können. Das heißt, die Atemwegsschleimhaut ist in der Lage, ein Nahrungsmittelallergen zu erkennen und gegebenenfalls eine allergische Reaktion in Gang zu setzen, vorausgesetzt, das Nahrungsmittelallergen steht inhalativ zur Verfügung.
Nahrungsmittelallergien: Sind sie „echt“ bzw. „primär“ oder eine Kreuzallergie?
Es gibt sowohl „primäre“, als auch „sekundäre“ Nahrungsmittelallergien. Etwa ¾ der Nahrungsmittelallergien sind sekundär. Das bedeutet, dass aerogene Allergene, zum Beispiel Pollen, über die Atemwege aufgenommen werden und mit ähnlichen Proteinen in Nahrungsmitteln kreuzreagieren. Circa 15 Prozent der Nahrungsmittelallergiker haben eine primäre Allergie. Hier erfolgt im Erwachsenenalter die Sensibilisierung im Magen-Darm-Trakt gegen relativ verdauungsstabile Proteine.
Hat die Psyche Auswirkungen auf eine Nahrungsmittelunverträglichkeit?
Der Zusammenhang zwischen psychischen Beschwerden bzw. Belastungsfaktoren und Nahrungsmittelallergien ist nur wenig erforscht. Es scheint jedoch direkte und indirekte Wechselwirkungen zu geben. In Stress-Situationen wird vom Körper Adrenalin ausgeschüttet, welches Mastzellen zur Ausschüttung von Histamin stimuliert. Umgekehrt ist eine chronische Belastung wie die einer allergisch bedingten Nahrungsmittelunverträglichkeit ein möglicher Auslöser oder Verstärker von Depressionen oder Angststörungen.
Nahrungsmittelallergie (NMA): Wie sehen die Symptome aus?
Die Symptome von Nahrungsmittelallergien und Nahrungsmittelunverträglichkeiten können an vielen Stellen des Körpers auftreten:
Allergiesymptome auf Nahrungsmittel manifestieren sich unter anderem:
- An der Haut
- An den Augen
- Am Darm
- Am Magen
- An der Speiseröhre
- An den Atemwegen
- Am Herz-Kreislauf-System
Allergische Reaktionen auf Nahrungsmittel sind also sehr vielfältig und können jedes Organ betreffen. Oft fragen sich die Patienten, wie sie eine Nahrungsmittelallergie erkennen können und was die ersten Anzeichen sind. Allergiesymptome können den Symptomen nicht allergisch bedingter Reaktionen sehr stark ähneln. Das ist einer der Gründe dafür, dass diese beiden völlig unterschiedlichen Erkrankungen in der öffentlichen Wahrnehmung häufig verwechselt bzw. „in einen Topf geworfen“ werden.
Pollenassoziierte Nahrungsmittelallergie oder Kreuzreaktionen
Bei pollenassoziierten Nahrungsmittelallergien ist das sogenannte Orale Allergiesyndrom sehr häufig. Es gehört also zur sekundären Nahrungsmittelallergie und weist eher milde Beschwerden auf. Die Betroffenen klagen nach dem Genuss von bestimmten Gemüse- und Obstsorten über ein pelziges Gefühl auf der Zunge, Juckreiz im Rachen, Lippenschwellung oder Bläschen auf der Zunge oder den Lippen. Die Beschwerden zeigen sich dann meist während der Pollensaison, können aber auch ganzjährig auftreten.
Was ist ein orales Allergiesyndrom?
Das Orale Allergiesyndrom ist die häufigste Nahrungsmittelallergie. Es ist die Folge einer Kreuzreaktion bei bestehender Pollenallergie oder Allergie auf Hausstaubmilben. Dann reagiert das Immunsystem nicht nur auf die Proteine in den Pollen oder im Kot der Hausstaubmilben, sondern auch auf „ähnlich aussehende Proteine“ in Nahrungsmitteln. Es kommt zu allergischen Reaktionen im Mund und Rachen. Man spricht dann von einem oralen Allergiesyndrom (OAS).
Die häufigsten auslösenden Nahrungsmittel für ein orales Allergiesyndrom sind:
- Äpfel
- Rohes Gemüse
- Karotten
- Sellerie
- Mandeln
- Nüsse
- Kiwi
- Kürbiskerne
- Hühnereiweiß
- Zitrusfrüchte
- Zimt
Kreuzreaktionen auf Nahrungsmittel bei Allergie auf Hausstaubmilben:
Hausstaubmilbenallergiker können Kreuzallergien gegenüber Krusten- und Schalentieren entwickeln. Grund dafür ist das Allergen Tropomyosin. Tropomyosin ist ein wichtiges Majorallergen welches in Meeresfrüchten und kommt in ähnlicher Struktur auch in Hausstaubmilben vor. Man spricht von einem Milben-Krustazeen-Mollusken-Syndrom. Es sind sogar schwere anaphylaktische Reaktionen möglich.
| Kreuzallergien bei Nahrungsmittelallergien und Inhalationsallergien | ||
| Allergen A | Allergen B (Kreuzallergen) | Häufigkeit |
| Kuhmilch | Ziegenmilch, Schafsmilch | Sehr häufig |
| Rindfleisch | Selten | |
| Stutenmilch, Kamelmilch | Sehr selten | |
| Hühnerei | Gänse-, Wachtel-, Entenei | Sehr häufig |
| Krustentiere (z.B.) | Andere Krustentiere (z.B.) | Häufig |
| Andere Meeresfrüchte, z.B. Muscheln, Tintenfisch, Rochen | Gelegentlich | |
| Fisch (z.B. Lachs) | Andere Fischsorten wie Scholle | Häufig |
| Geflügelfleisch | Gelegentlich | |
| Schwertfisch, Thunfisch, Rochen | Selten | |
| Nuss (z.B. Walnuss) | Andere Baumnüsse, wie Haselnuss oder Cashewnuss | Häufig |
| Pekanuss | Sehr häufig | |
| Erdnuss | Hülsenfrüchte wie Lupine oder Soja | Selten |
| Andere Hülsenfrüchte wie Linsen, Erbsen, Kichererbsen, Bohnen | Sehr selten | |
| Cashew | Pistazie | Sehr häufig |
| Soja | Erdnuss, Hülsenfrüchte | Gelegentlich |
| Getreide | Andere Getreidearten (Gerste, Roggen, Mais) | Gelegentlich |
| Rotes Fleisch (wie Schwein, Rind, Lamm) | Schweineschmalz, Gelatine, Innereien | Häufig |
| Geflügelfleisch | Fisch | Selten |
| Lipidtransferproteine (Majorallergen vieler pflanzlicher Lebensmittel) | Kern- und Steinobst, Nüsse | Häufig |
| Kiwi, Banane, Beerenobst | Gelegentlich | |
| Tomate, Paprika, Gurke, Mais, Mohn, Samen wie Sonnenblumenkerne | Selten | |
| Quelle: Dr. med. Anna Eger, www.mein-allergie-portal.com | ||
Symptome bei echten, primären Nahrungsmittelallergien:
Nicht selten kann es bei Allergien gegen Nahrungsmittel zu systemischen Reaktionen kommen, die sich auf den ganzen Körper ausbreiten.
Symptome bei echten, IgE-vermittelten Nahrungsmittelallergien sind zum Beispiel:
An Haut und Schleimhaut:
- Urtikaria – Nesselsucht - Hautausschlag, oft juckend
- Angioödem – Schwellungen, oft juckend
- Flush – anfallsartige Rötung der Haut
- Kribbeln, Brennen, Juckreiz im Mund, an Lippen oder Zunge beim OAS
An den Augen:
- Juckreiz
- Rötung
- Tränenfluss
- Lidschwellung
Am Magen-Darm-System
- Bauchschmerzen
- Magenschmerzen
- Übelkeit
- Erbrechen
- Durchfall
- Verstopfung
- Blutige Stühle
An den Atemwegen
- allergische Rhinokonjunktivitis – Heuschnupfen
- allergisches Asthma
- Kehlkopfschwellung mit pfeifendem Atemgeräusch
- Heiserkeit
Am Herz-Kreislauf-System
- Müdigkeit
- Erschöpfung
- Blutdruckabfall
- Kreislaufzusammenbruch
- anaphylaktischer Schock
Allergischer Schock auf Lebensmittel: Wie können die Symptome aussehen?
Bei der schwersten Form der Nahrungsmittelallergie, der Anaphylaxie, kann es zu sehr unterschiedlichen Symptomen kommen. Eine Anaphylaxie ist ein sogenanntes Multiorgangeschehen, das bedeutet es kann nicht nur zu Symptomen an der Haut, wie Urtikaria, oder auch zu Rötungen und Juckreiz kommen. Hinzu kommen weitere Symptome an den Atemwegen wie Luftnot, dem Verdauungssystem wie Darmkrämpfe oder Erbrechen und dem Kreislauf bis hin zum Kreislaufversagen.
Was ist eine verzögerte Nahrungsmittelallergie?
Im Gegensatz zur Allergie vom Sofort-Typ, der Typ-I-Allergie, die über IgE-Antikörper ausgelöst wird, wird die verzögerte Nahrungsmittelallergie durch andere Antikörper, die IgG, oder andere Mechanismen vermittelt. Sie zählt man zur Allergie Typ II bis Typ IV. Diese Form der Nahrungsmittelallergie ist schwieriger zu erkennen, obwohl sie eigentlich deutlich häufiger vorkommt. Dazu gehört, dass es nicht so einfach ist, sie zu diagnostizieren, denn es gibt keinen Bluttest und auch keinen sicher etablierten Hauttest. Wie der Name schon sagt, treten die Symptome einer verzögerten Nahrungsmittelallergie erst Stunden oder sogar Tage nach dem Verzehr auf. Somit wird oftmals gar kein Bezug zum verursachenden Lebensmittel festgestellt.
Fleischallergie - Alpha-Gal-Syndrom (AGS)
Allergien auf Säugetierfleisch äußern sich ebenfalls erst verzögert mit Urtikaria und teilweise schweren anaphylaktischen Reaktionen, sie sind aber IgE-vermittelt. Für die allergische Reaktion verantwortlich ist die sogenannte alpha-Galaktosidase. In den letzten Jahren hat man festgestellt, dass eine Allergie gegen rotes Fleisch durch Zeckenbisse ausgelöst werden kann.
WDEIA (Weizenabhängige anstrengungsinduzierte Anaphylaxie)
Eine Sonderform der Weizenallergie ist die Weizenabhängige anstrengungsinduzierte Anaphylaxie (WDEIA). Hierbei treten anaphylaktische Reaktionen nach dem Verzehr von weizenhaltigen Lebensmitteln erst in Verbindung mit körperlicher Anstrengung auf. In Ruhe hingegen werden Weizenhaltige Lebensmittelvertragen. Die klinischen Symptome einer anstrengungsinduzierten Anaphylaxie entsprechen den Symptomen der Anaphylaxie allgemein. Ganz oft bleiben Menschen, die an einer WDEIA leiden, über lange Zeiträume hinweg beschwerdefrei. Zur anaphylaktischen Reaktion kommt es bei von WDEIA Betroffenen immer nur dann, wenn der Weizenverzehr, meist innerhalb von 30 Minuten bis 2 Stunden, nach dem Verzehr mit einem Verstärkungsfaktor zusammentrifft. Der häufigste Verstärkungsfaktor bei der WDEIA ist körperliche Aktivität. Die Menge des verzehrten Weizens spielt dabei keine Rolle. Auch kleinste Weizenmengen können eine WDEIA auslösen.
Eosinophile Ösophagitis (EoE): wie sehen die Symptome aus?
Die meisten Patienten mit eosinophiler Ösophagitis leiden schon mehrere Jahre, bevor die Diagnose gestellt wird, an Schluckbeschwerden: Vor allem bei festen Speisen müssen sie häufig würgen, auch wenn sie sorgfältig kauen. Der Speisebrei lässt sich nicht einfach schlucken, sondern bleibt auf dem Weg in den Magen immer wieder stecken. Sobald die Speiseröhre wieder frei ist, sind die Beschwerden vorüber. Die Betroffenen essen meist sehr vorsichtig, kauen intensiv, trinken regelmäßig während des Essens. Dennoch kommt es immer wieder zu den Schluckbeschwerden. Etwa die Hälfte der Patienten mit EoE klagt zudem über Brennen hinter dem Brustbein. Im Gegensatz zu Sodbrennen wie bei der Refluxkrankheit steigt der Schmerz aber nicht vom Magen aus auf. Typischerweise kommt es im Verlauf auch wiederholt zu einer akuten Blockade der Speiseröhre: Ein Stück Nahrung bleibt stecken und lässt sich weder hochwürgen noch herunterschlucken. Da dies häufig beim Verzehr von Fleisch passiert, nennen Ärzte es auch „Steakhouse-Syndrom“ oder auch „Bolusobstruktion der Speiseröhre“.
Food Protein-Induced Enterocolitis Syndrome (FPIES): Wie sehen die Symptome aus?
Eine weitere Sonderform der Nahrungsmittelallergien ist das „Food Protein-Induced Enterocolitis Syndrome“, kurz „FPIES“ genannt. Der Mechanismus hinter einem FPIES geht in Richtung Allergie vom Spättyp, die nicht IgE-vermittelt wird. Man weiß aber aktuell noch nicht genau, wie der genaue Ablauf der Entzündungsreaktion ist.
Etwas 1 bis 4 Stunden nach dem Verzehr des auslösenden Nahrungsmittels kommt es zu:
- wiederholtem Erbrechen
- Durchfall
- Dadurch bedingtem massiven Flüssigkeitsverlust
- Evtl. Fieber
- Anaphylaktischen Reaktionen
Bei Kindern kommen Gewichtsverlust und Wachstumsstörungen hinzu.
Nicht IgE-vermittelte Nahrungsmittelallergie: Wie sehen die Symptome aus?
Die Symptome einer verzögerten Nahrungsmittelallergie, die nicht über IgE vermittelt wird, äußern sich vor allem in:
- Übelkeit
- Erbrechen
- Bauchschmerzen
- Sodbrennen
- Appetitlosigkeit
- Durchfall
- Blutiger Stuhlgang
- Gedeihstörungen
- Gewichtsverlust
Wie lange dauert eine allergische Reaktion auf Lebensmittel?
Wie lange eine allergische Reaktion nach Kontakt bzw. Verzehr mit dem auslösenden Lebensmittel andauert, kann man nicht pauschal sagen und auch nicht abschätzen. Bei Allergien vom Sofort-Typ treten die Symptome in der Regel relativ rasch auf und können von Minuten bis einige Stunden anhalten. Je nachdem, ob und welche Akuttherapie ggf. eingeleitet wird, sollte die Reaktion spätestens innerhalb einiger Stunden wieder verschwunden sein.
Kann eine Nahrungsmittelallergie zu einem Vitaminmangel führen?
In einigen seltenen Fällen kann es beispielsweise durch multiple Unverträglichkeiten oder auch bei der Notwendigkeit einer strikten Eliminationsdiät bzw. bei vorliegenden Begleiterkrankungen zu einer unzureichenden Zufuhr von Vitaminen kommen. Allerdings gibt es keine allgemeine Empfehlung zur Supplementierung von Vitaminen. Normalerweise sollte eine ausreichend vitaminhaltige Ernährung möglich sein.
Ist es üblich, dass es bei einer Nahrungsmittelallergie zu einer Gewichtszunahme bzw. Gewichtsabnahme führt?
Bei einigen, besonders den nicht IgE-vermittelten, Nahrungsmittelallergien, kann es bei schweren oder langfristigen Verlaufsformen zu Gewichtsverlust kommen. Eine Nahrungsmittelallergie als Ursache für eine Gewichtszunahme ist eher unwahrscheinlich.
Nahrungsmittelallergien beim Kind
Auch Kinder können von einer Nahrungsmittelallerig betroffen sein. Eine Nahrungsmittelallergie beim Kind muss aber nicht dauerhaft bestehen bleiben. Bei den meisten Kindern verliert sie sich bis zum Schulalter wieder. Wie die Allergien beim Kind entstehen, ist noch nicht vollständig erforscht.
Haben Babys auch schon Lebensunverträglichkeiten oder entwickeln sich Nahrungsmittelallergien erst im Alter?
Etwa 5 bis 10 Prozent der IgE-vermittelten Nahrungsmittelallergien treten bereits im Säuglingsalter auf. Die gute Nachricht ist aber, dass sich mit Ausreifung der oralen Toleranz die Allergie bei etwa 80 Prozent wieder zurückbildet. Verantwortliche Allergene für Allergien im Säuglingsalter sind stabile Proteine aus Milch, Ei, Fisch, Erdnuss, Haselnuss und Soja.
Auch das FPIES tritt überwiegend bei Säuglingen und Kleinkindern auf. Ein weiteres Beispiel für Nahrungsmittelallergien bei Babys ist die nahrungsmittelproteininduzierte Enteropathie.
Anaphylaktische Reaktion bei Kindern
70 bis 80 Prozent der Kinder haben im Rahmen einer IgE-vermittelten allergischen Frühreaktion Symptome an der Haut.
Häufig kann es bei Kindern bei allergischen Reaktionen auf Nahrungsmittel zu Reaktionen an den Atemwegen, das heißt zu einer Asthmasymptomatik kommen. Das ist auch bei Kindern möglich, die kein Asthma haben. Aber auch Symptome wie ein Larynxödem, eine Schwellung am Kehlkopf, Husten und Heiserkeit können im Rahmen eines anaphylaktischen Schocks auftreten.
Oft kommt es zu Symptomen am Magen-Darm-Trakt, wie Übelkeit oder Bauchschmerzen. Bei einer schweren Reaktion können die Schmerzen Kolik-artig auftreten. Als Erstsymptom ist bei Kindern Erbrechen sehr häufig. Mit einer gewissen Verzögerung kann das Kind auch Durchfall bekommen.
Bei einer schweren allergischen Reaktion oder Anaphylaxie kann es zu Blutdruckabfall, Kollaps oder Bewusstlosigkeit kommen. Diese Reaktion ist jedoch im Kindesalter deutlich seltener als bei Erwachsenen. Es gibt bei der Anaphylaxie aber auch sehr unspezifische Symptome.
Untypische Symptome einer Anaphylaxie bei Kindern
Ein sehr häufiges unspezifisches Symptom bei kindlichen Anaphylaxien, das oft auch ein Initialsymptom ist, ist der Juckreiz an Mund oder Rachen. Das Problem ist, dass kleine Kinder dieses Symptom oft nicht gut kommunizieren können. Manchmal fassen sie sich dann an den Mund, versuchen den Mund auszuspülen oder spucken die Lebensmittel aus. Das kann ein erstes Warnzeichen sein, ist jedoch sehr unspezifisch, denn kleine Kinder machen dies oft auch dann, wenn sie ein Nahrungsmittel einfach nicht mögen.
Eosinophile Ösophagitis bei Kindern
Bei Kindern zeigt sich die eosinophile Ösophagitis häufig eher darin, dass sie ungern essen oder die Nahrung ganz verweigern. Hinzu können Gedeih- bzw. Wachstumsstörungen kommen. Viele Kinder mit eosinophiler Ösophagitis haben zudem Schmerzen im Bereich der Brust oder des Bauchs. Sie erbrechen bzw. würgen Nahrung hoch und haben Durchfall.
Diagnose von Nahrungsmittelallergien
Die Diagnosestellung einer NMA erfolgt durch eine Kombination verschiedener diagnostischer Methoden. Dazu gehören die ausführliche Anamnese durch Arzt und Ernährungsfachkraft. Allergietests auf Nahrungsmittelallergien werden als Hauttests in Form eines Prick-Tests und als Bluttests in Form von IgE-Tests oder molekularer Allergiediagnostik durchgeführt. Auch eine diagnostische Diät, das ist eine Eliminationsdiät, mit Ernährungs- und Symptomtagebuch, und eine orale Provokation können zur Diagnose einer Nahrungsmittelallergie dazu gehören.
Zu beachten ist, dass es sich bei einem positiven Haut- und Bluttest noch nicht um eine Allergie handelt, sondern lediglich um eine Sensibilisierung. Die orale Provokation soll dann zeigen, ob das vermutete Lebensmittel tatsächlich auch Reaktionen auslöst. Hier ist der Goldstandard der doppelblind-placebo-kontrollierte Provokationstest, der leider nur sehr selten durchgeführt wird.
Kann man bei Nahrungsmittelallergien auch eine Diagnose ohne Eliminationsdiät stellen?
Das Durchführen einer Eliminationsdiät ist im Rahmen der Diagnostik auf Nahrungsmittelallergien zwar oft hilfreich, aber nicht zwingend erforderlich. In einigen Fällen sollte sie sogar vermieden werden.
Was ist ein IgG-Test auf Nahrungsmittel?
Ein IgG-Test ist kein Nahrungsmittelallergie-Test. Dieser Bluttest hat keinerlei Aussagekraft im Hinblick auf Allergien oder Intoleranzen.
Therapie bei Nahrungsmittelallergien
Welche Therapie bei einer Allergie auf Lebensmittel die richtige ist, hängt von der Ursache ab.
Allgemeine Therapie bei echter Nahrungsmittelallergie
Nach bestätigter Diagnose besteht bei einer Nahrungsmittelallergie die einzige Therapie in einem konsequenten Vermeiden des auslösenden Allergens. Zusammen mit einer Ernährungsfachkraft wird dann mit dem Betroffenen eine auf ihn abgestimmte Ernährung gefunden, die zum einen die Lebensqualität erhalten und zum anderen einer Unterversorgung entgegenwirken soll.
Betroffene mit einer ausgeprägten Allergie sowie Personen, die bereits eine anaphylaktische Reaktion auf ein Nahrungsmittel gezeigt haben, sollten ein Notfall-Medikamentenset, bestehend aus einem Antihistaminikum, einem Glucocorticoid (Cortison) und einem Adrenalin Autoinjektor, bei sich tragen. Außerdem gehört ein Schulungsprogramme für die Betroffenen zum Therapiekonzept.
Als medikamentöse Dauertherapie gibt es keine allgemeine Therapieempfehlung für bestimmte antiallergische Medikamente.
Immunologische Therapie bei Nahrungsmittelallergien
Bei primären Nahrungsmittelallergien wurde versucht, mithilfe verschiedener Formen der Immuntherapie zu behandeln. Diese sind die:
- subkutane Immuntherapie (SCIT)
- sublinguale Immuntherapie (SLIT)
- orale spezifische Immuntherapie (OIT)
- epikutane Immuntherapie (EPIT)
Allerdings ist die Bewertung der Studien zur Immuntherapie bei Nahrungsmittelallergien schwierig. In bestimmten Fällen, wie zum Beispiel bei einer pollenassoziierten Nahrungsmittelallergie, kann sie jedoch unter bestimmten Bedingungen in Erwägung gezogen werden.
Gibt es eine Therapie bei Allergie auf Erdnuss?
Die Allergene der Erdnuss gehören zu den gefährlichsten Allergenen. Die allergischen Reaktionen können sehr gravierend sein, bis hin zum anaphylaktischen Schock. Das Risiko, versehentlich mit dem Erdnussallergen in Kontakt zu kommen, ist sehr hoch. Eine orale spezifische Immuntherapie scheint eine Behandlungsoption zu sein, bei der gut 50 Prozent der Erdnuss-Allergiker eine Toleranz gegen Erdnuss erreichen. Außerdem wird an einer epikutanen Immuntherapie geforscht, bei der eine Art „Erdnusspflaster“ auf die Haut aufgeklebt wird. Seit Mitte 2021 gibt es ein zugelassenes Therapeutikum für Erdnussallergiker, das oral verabreicht wird. In seiner Pressemitteilung „Hyposensibilisierung mit AR101 bei Erdnussallergie: Beleg für einen geringeren Nutzen“ vom 17.1.2022 kam das Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen (IQWiG) jedoch zu der folgenden Bewertung: „In den patientenrelevanten Endpunkten gibt es für 4- bis 17-Jährige ausschließlich Nachteile gegenüber einer reinen erdnussvermeidenden Diät. Nur in einem artifiziellen Surrogatendpunkt zeigt sich ein Vorteil“. (Quelle: https://www.iqwig.de/projekte/a21-135.html) Es befindet sich außerdem ein Erdnussallergoidextrakt zur Therapie der Erdnussallergie in Entwicklung, dass besser verträglich sein soll. Es gibt auch Therapieansätze mit Biologika wie Omalizumab oder Etokimab.
Ligelizumab zur Therapie bei Nahrungsmittel-Allergien: Woran wird geforscht?
Zur Behandlung einer IgE-vermittelten Allergie auf Erdnüsse wurde 2022 eine Phase-III-Studie zu Ligelizumab begonnen.Der monoklonale, humanisierte Anti-IgE-Antikörper Ligelizumab hemmt spezifisch den IgE-/FcεRI-Signalweg und blockiert IgE-vermittelte Reaktionen unter Beteiligung des hochaffinen IgE-Rezeptors FcRI, dessen Aktivierung durch das Allergen eine zentrale Rolle bei Nahrungsmittelallergien spielt. Der Wirkstoff wird entwickelt zur Risikoreduktion von allergischen Symptomen und Anaphylaxien. Diese Effekte sind derzeit Gegenstand der klinischen Untersuchungen.
In die Studie eingeschlossen wurden von einer IgE-vermittelten Allergie auf Erdnuss betroffene Menschen zwischen 12 und 55 Jahren. Ziel dieser randomisierten, doppelblinden, placebo-kontrollierten Studie ist die Untersuchung der Sicherheit und klinischen Wirksamkeit von zwei Wirkstoff-Dosierungen (240 mg oder 120 mg, alle 4 Wochen) in insgesamt 5 Behandlungsarmen im Vergleich zu Placebo. Insgesamt sollen 486 Studienteilnehmerinnen und -teilnehmer mit einer medizinisch bestätigten Diagnose der IgE-vermittelten Nahrungsmittelallergie gegen Erdnüsse über einen Zeitraum von 52 Wochen behandelt und weitere 16 Wochen nachbeobachtet werden. Die Behandlung erfolgt per subkutaner Injektion, das heißt durch eine Spritze, in vierwöchigen Abständen. Das voraussichtliche Studienende ist für 2025 geplant.
Primärer Studienendpunkt, also Ziel der Studie, ist die Untersuchung der Wirksamkeit der Prüfsubstanz im Vergleich zu Placebo. Dies gemessen am Anteil der Patientinnen und Patienten, die eine Einzeldosis von ≥ 600 mg (1.044 mg kumulativ verträgliche Dosis) Erdnussprotein ohne dosislimitierende Symptome während der doppelblinden, placebo-kontrollierten, oralen Nahrungsmittelprovokation am Ende der 12-wöchigen Behandlung tolerieren können.
Entsprechende weitere Studien zur Wirksamkeit und Verträglichkeit von Ligelizumab bei Allergien gegen Milch und Ei befinden sich bereits in der Planung.
Therapie bei pollenassoziierter Kreuzallergie auf Nahrungsmittel
Bei einer pollenassoziierten Nahrungsmittelallergie (Kreuzallergie) treten Symptome häufig nur bei Verzehr von rohem Gemüse und Obst auf. Beispielsweise vertragen Birkenpollenallergiker, die auf rohen Apfel mit einem Oralen Allergiesyndrom reagieren, diesen in Form von Apfelmus oder Apfelkuchen. Allergene in Nüssen, Kräutern und Gewürzen sind jedoch auch hitzestabil und rufen auch nach dem Erhitzen Symptome hervor.
Die Stärke des Pollenfluges kann ebenfalls Einfluss auf die Symptome haben. Zum Teil führen Lebensmittel nur zur entsprechenden Pollenflugzeit zu Beschwerden, oder die Reaktionen sind dann deutlich stärker. Das Spektrum der unverträglichen Nahrungsmittel kann sich mit der Zeit ausweiten. Es macht aber keinen Sinn bei einer pollenassoziierten Nahrungsmittelallergie vorbeugend alle möglichen kreuzreaktiven Nahrungsmittel zu meiden. Nur diejenigen Nahrungsmittel, bei denen sich auch Symptome zeigen, sollte aus dem Speiseplan entfernt werden.
Therapie bei Kreuzallergie auf Milben
Bei Nahrungsmittelallergikern, die außerdem eine Kreuzallergie auf Milben haben, sollte außer dem Meiden der auslösenden Lebensmittel zusätzlich eine gründliche Milbensanierung im Wohnumfeld durchgeführt werden. Außerdem ist die Indikation für eine spezifische Immuntherapie gegen Hausstaubmilben zu prüfen. Auch das Ausstellen eines Notfallsets muss bei einem vorangegangenen anaphylaktischen Ereignis erfolgen.
Lässt sich eine Lebensmittallergie heilen?
Das Meiden des auslösenden Allergens ist der wichtigste therapeutische Faktor nach der Diagnose einer Nahrungsmittelallergie. Davon ist der Betroffene jedoch nicht geheilt. Beim nächsten Verzehr oder Kontakt mit dem entsprechenden Lebensmittel ist eine erneute Reaktion zu erwarten. Eine medikamentöse Heilung der Nahrungsmittelallergie gibt es leider nicht. Jedoch gibt es mit der oralen Immuntherapie neue Perspektiven um eine klinische Toleranz zu erreichen.
Gibt es eine natürliche Behandlung gegen Nahrungsmittelallergien?
Viele Patienten, egal mit welcher Erkrankung, sind zunehmend auf der Suche nach milden, verträglichen, nebenwirkungsarmen Behandlungsmethoden. So auch im Fall von Nahrungsmittelallergien. Von Heilpraktikern bzw. Homöopathen werden die verschiedensten Möglichkeiten und Präparate angeboten. Bisher hat jedoch keine dieser alternativen Heilmethoden oder homöopathischen Mittel in Studien mit ihrer Wirksamkeit überzeugt und gehört deshalb nicht in die leitliniengerechte Therapie.
Nahrungsmittelallergie – kann man vorbeugen?
Es gibt verschiedene Empfehlungen, wie man bestimmten Nahrungsmittelallergien vorbeugen kann.
In Bezug auf Hühnerei beispielsweise wurde in Studien gezeigt, dass das Einführen von durcherhitztem Hühnerei – also verbacken oder gekocht – mit der Beikost günstige Effekte auf die Vermeidung einer Hühnerei-Allergie hat, während allerdings pasteurisiertes Vollei das Risiko anaphylaktischer Reaktionen erhöhe.
Für die Erdnussallergie existieren ebenfalls Daten, die besagen, dass das regelmäßige Füttern eines Säuglings in Familien mit erhöhter Atopieneigung mit Erdnussbutter zur Reduktion des Risikos einer Erdnussallergie führt. Allerdings sollte bei Babys mit einer mittelschweren oder schweren atopischen Dermatitis zuerst eine Erdnussallergie ausgeschlossen werden.
Weitere Empfehlungen um Nahrungsmittelallergien vorzubeugen sind:
- ausgewogene Ernährung während Schwangerschaft und Stillzeit ohne Meidung potentieller Nahrungsmittelallergiequellen
- ausschließliches Stillen für die ersten 4 bis 6 Lebensmonate, wenn möglich
- wenn möglich, auf kuhmilchbasierte Formulanahrung in den ersten Lebenstagen verzichten
- wenn ein Säugling nicht gestillt wird, geeignete Säuglingsanfangsnahrung verabreichen, keine soja-basierte Säuglingsnahrung verwenden
- vielfältige Säuglingsnahrung zwischen dem 5. Und dem 7. Lebensmonat einführen, einschließlich Fisch, Milch, Naturjoghurt und Hühnerei
Bei welchem Arzt kann man eine Nahrungsmittelallergie testen lassen?
Tests zu Nahrungsmittelallergien werden von einem Allergologen durchgeführt. Allergologie ist eine Zusatzqualifikation, die vor allem Hautärzte, HNO-Ärzte und Lungenfachärzte haben. Jedoch können auch Kinderärzte, Internisten und Allgemeinärzte eine solche Zusatzbezeichnung tragen. Wer den Verdacht hat, an einer Nahrungsmittelallergie zu leiden, der stellt sich am besten bei seinem Hausarzt vor und dieser wird bei entsprechender Notwendigkeit zu einem entsprechenden Facharzt überweisen.
Kann eine Nahrungsmittelallergie von selbst verschwinden?
Eine Nahrungsmittelallergie vom Typ A, die im Säuglingsalter auftritt, kann sich im Laufe der Jahre zurückentwickeln. Bei etwa drei Viertel der betroffenen Kleinkinder verliert sich die Nahrungsmittelallergie in den ersten Lebensjahren wieder, so dass regelmäßig etwa alle 1 bis 2 Jahre unter ärztlicher Aufsicht überprüft werden sollte, ob sie noch relevant ist. Eine Erdnuss-, Baumnuss-, Fisch- und Krebstierallergie wird bis ins Erwachsenenalter bestehen bleiben.
Quellen:
dgaki.de/wp-content/uploads/2022/02/Worm-2021-Update-Leitlinie-Management-IgE-vermittelter-Nahrungsmittelallergien-1.pdf
Deutsches Ärzteblatt: Archiv "Nahrungsmittelallergien: Allergene essen, statt meiden" (05.10.2018) (aerzteblatt.de)
www.aerzteblatt.de/archiv/179902/Mikrobiom-Forschung-Kann-die-Darmflora-Allergien-verhindern
www.aerzteblatt.de/archiv/195370/Nahrungsmittelallergie-Wenn-das-Essen-krank-macht
www.aerzteblatt.de/archiv/64730/Differenzialdiagnose-von-Nahrungsmittelunvertraeglichkeiten
www.altmeyers.org/de/allergologie/nahrungsmittelallergie-2682
www.altmeyers.org/de/allergologie/allergiesyndrom-orales-4769
www.altmeyers.org/de/allergologie/milben-krustazeen-mollusken-syndrom-15413
www.altmeyers.org/de/allergologie/weizenabhangige-anstrengungsinduzierte-anaphylaxie-16299
www.altmeyers.org/de/gastroenterologie-hepatologie/eosinophile-osophagitis-24349
www.altmeyers.org/de/allergologie/enterokolitissyndrom-nahrungsmittelprotein-induziertes-26429
www.iqwig.de/projekte/a21-135.html
vaem.eu/wissensdatenbank/diagnose/definition/
Medienmitteilung, Novartis startet erste Phase-III-Studie mit Ligelizumab (QGE031) zur Prävention bei IgE-vermittelter Nahrungsmittelallergie in Deutschland, 27.7.2022
Wichtiger Hinweis
Unsere Beiträge beinhalten lediglich allgemeine Informationen und Hinweise. Sie dienen nicht der Selbstdiagnose, Selbstbehandlung oder Selbstmedikation und ersetzen nicht den Arztbesuch. Die Beantwortung individueller Fragen durch unsere Experten ist leider nicht möglich.
Autor: A. Eger, mein-allergie-portal.com
Lesen Sie auch
-
Allergiesymptome durch Nahrungsmittel? Kreuzallergie auf Frühblüher?
-
Allergisch auf Nüsse! Auch auf Muskatnuss, Kokosnuss & co.?
-
Allergie auf Sesam: Ein unterschätztes Risiko?
Weitere Beiträge
News - Nahrungsmittelallergie und -unverträglichkeiten
- Allergisch auf Erdbeeren, gibt es das?
- Allergie auf Tomaten: Symptome & Maßnahmen
- Eosinophile Ösophagitis durch Reinigungsmittel?
- Sulfit-Intoleranz: Was kann man noch essen?
- Alpha-Gal-Syndrom? Fleischallergie? Symptome & Risiken
- Soja Unverträglichkeit - Soja Allergie: Was essen?
- Stiller Reflux: Ursachen, Symptome, Therapie
- FPIES: Ursachen, Symptome, Diagnose und Therapie
MeinAllergiePortal wird unterstützt von